Page 400 - SAHCS HIVMed Journal Vol 20 No 1 2019
P. 400
Page 5 of 7 Original Research
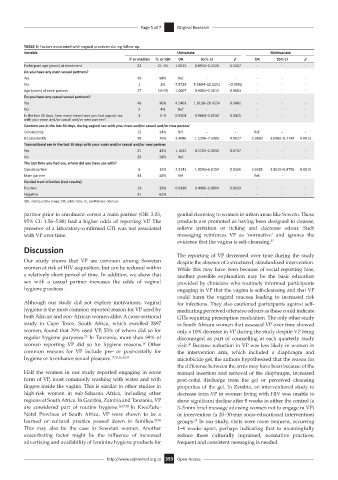
TABLE 3: Factors associated with vaginal practices during follow-up.
Variable Univariate Multivariate
N or median % or IQR OR 95% CI p OR 95% CI p
Participant age (years) at enrolment 22 21–24 1.0535 0.8933–1.2426 0.5357 - - -
Do you have any main sexual partners?
Yes 49 98% Ref. - - - - -
No 1 2% 7.8729 5.5694–11.1291 <0.0001 - - -
Age (years) of main partner 27 24–29 1.0007 0.9092–1.1014 0.9883 - - -
Do you have any casual sexual partners?
Yes 48 96% 4.5461 1.0118–20.4254 0.0482 - - -
No 2 4% Ref - - - - -
In the last 30 days, how many times have you had vaginal sex 3 2–3 0.9904 0.9664–1.0150 0.4421 - - -
with your main and/or casual and/or new partner?
Condom use in the last 30 days, during vaginal sex with your main and/or casual and/or new partner
Consistently 12 24% Ref. - - Ref. - -
Inconsistently 38 76% 3.4086 1.5306–7.5906 0.0027 3.3860 1.6980–8.7748 0.0013
Transactional sex in the last 30 days with your main and/or casual and/or new partner
Yes 21 42% 1.1635 0.5723–2.3656 0.6757 - - -
No 29 58% Ref. - - - - -
The last time you had sex, whom did you have sex with?
Casual partner 6 12% 2.5242 1.0593–6.0154 0.0366 3.0285 1.5610–5.8756 0.0010
Main partner 44 88% Ref. - - Ref. - -
Genital tract infection (test results)
Positive 19 38% 0.9189 0.4490–1.8804 0.8169 - - -
Negative 31 62% - - - - - -
IQR, interquartile range; OR, odds ratio; CI, confidence interval.
partner prior to enrolment versus a main partner (OR: 3.03, genital cleansing to women in urban areas like Soweto. These
95% CI: 1.56–5.88) had a higher odds of reporting VP. The products are promoted as having been designed to cleanse,
presence of a laboratory-confirmed GTI was not associated relieve irritation or itching and decrease odour. Such
with VP over time. messaging reinforces VP as ‘normative’ and ignores the
evidence that the vagina is self-cleansing.
37
Discussion
The reporting of VP decreased over time during the study
Our study shows that VP are common among Sowetan despite the absence of a structured, standardised intervention.
women at risk of HIV acquisition, but can be reduced within While this may have been because of social reporting bias,
a relatively short period of time. In addition, we show that another possible explanation may be the basic education
sex with a casual partner increases the odds of vaginal provided by clinicians who routinely informed participants
hygiene practices. engaging in VP that the vagina is self-cleansing and that VP
could harm the vaginal mucosa leading to increased risk
Although our study did not explore motivations, vaginal for infections. They also cautioned participants against self-
hygiene is the most common reported reason for VP used by medicating perceived offensive odours as these could indicate
both African and non-African women alike. A cross-sectional GTIs requiring prescription medication. The only other study
study in Cape Town, South Africa, which enrolled 2897 in South African women that assessed VP over time showed
women, found that 29% used VP, 53% of whom did so for only a 10% decrease in VP during the study despite VP being
regular hygiene purposes. In Tanzania, more than 99% of discouraged as part of counselling at each quarterly study
23
women reporting VP did so for hygiene reasons. Other visit. Because reduction in VP was less likely in women in
16
30
common reasons for VP include pre- or post-coitally for the intervention arm, which included a diaphragm and
hygiene or to enhance sexual pleasure. 17,25,26,33,34 microbicide gel, the authors hypothesised that the reason for
the difference between the arms may have been because of the
Half the women in our study reported engaging in some manual insertion and removal of the diaphragm, increased
form of VP, most commonly washing with water and with post-coital discharge from the gel or perceived cleansing
fingers inside the vagina. This is similar to other studies in properties of the gel. In Zambia, an interventional study to
high-risk women in sub-Saharan Africa, including other decrease intra-VP in women living with HIV was unable to
regions of South Africa. In Gambia, Zambia and Tanzania, VP show significant decline after 8 weeks in either the control (a
are considered part of routine hygiene. 16,17,35 In KwaZulu- 3–5-min brief message advising women not to engage in VP)
Natal Province of South Africa, VP were shown to be a or intervention (a 20–30-min socio-educational intervention)
learned or cultural practice passed down in families. 29,36 groups. In our study, visits were more frequent, occurring
35
This may also be the case in Sowetan women. Another 1–4 weeks apart, perhaps indicating that to meaningfully
exacerbating factor might be the influence of increased reduce these culturally ingrained, normative practices,
advertising and availability of feminine hygiene products for frequent and consistent messaging is needed.
http://www.sajhivmed.org.za 393 Open Access